- Case-Based Roundtable
- General Dermatology
- Eczema
- Chronic Hand Eczema
- Alopecia
- Aesthetics
- Vitiligo
- COVID-19
- Actinic Keratosis
- Precision Medicine and Biologics
- Rare Disease
- Wound Care
- Rosacea
- Psoriasis
- Psoriatic Arthritis
- Atopic Dermatitis
- Melasma
- NP and PA
- Skin Cancer
- Hidradenitis Suppurativa
- Drug Watch
- Pigmentary Disorders
- Acne
- Pediatric Dermatology
- Practice Management
- Prurigo Nodularis
- Buy-and-Bill
News
Article
Many Patients With Moderate to Severe AD Demonstrate Inadequate Disease Control with Systemic Therapies After 3 to 12 Months of Use
Author(s):
The study findings were presented in a poster at the 2023 Revolutionizing Atopic Dermatitis Virtual Conference.
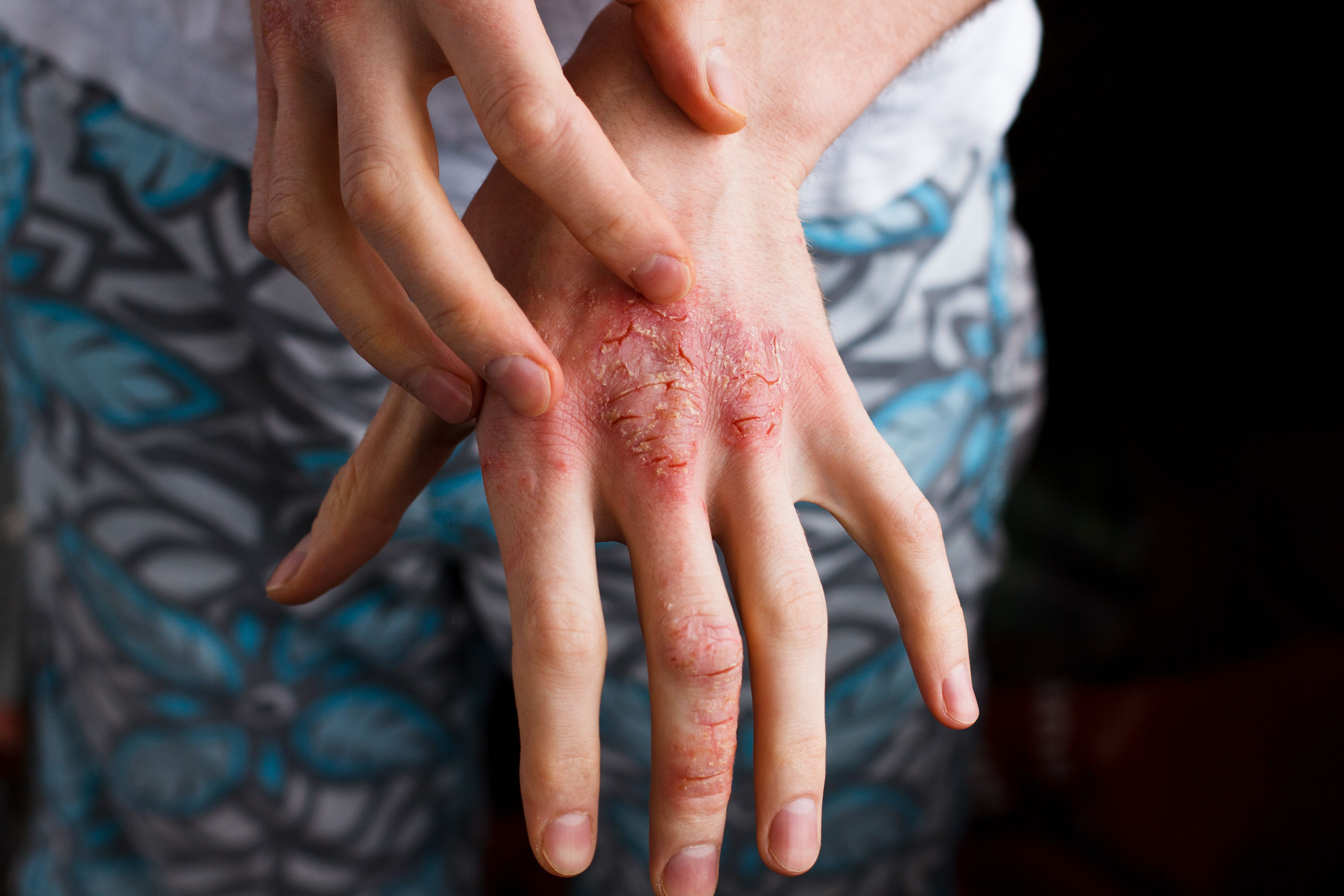
Study authors of a poster from the Revolutionizing Atopic Dermatitis Virtual Conference, held December 10, 2023, found that many patients with moderate to severe atopic dermatitis (AD) do not achieve adequate disease control with systemic therapies over 12 months. Eichenfield et al noted that their findings suggest a “substantial presence of therapeutic inertia.”
According to the authors, therapeutic inertia is the delay or failure of timely adjustment to therapy when treatment goals are not met, which further complicates the management of moderate to severe AD. “Despite the availability of conventional (CST) and advanced systemic therapies (AST) currently utilized for the treatment of moderate to severe AD, many patients do not achieve treatment success,” wrote Eichenfield et al. CST therapies included methotrexate, cyclosporine, mycophenolate mofetil, azathioprine, and systemic corticosteroids, whereas AST therapies included abrocitinib, dupilumab, tralokinumab, or upadacitinib.
The study authors acknowledged that the extent of why patients do not achieve disease control with systemics after 12 months requires further research.
Eichenfield et al conducted a longitudinal analysis of patients with moderate to severe AD (a Validated Investigator Global Assessment for Atopic Dermatitis (vIGA-AD) score of ≥3) from the TARGET-DERM AD registry, including 3457 patients from 39 centers in the US and Canada. Patients eligible for the study had documented outcomes at the initiation of systemic therapy, and after 3 months up to 12 months of follow up and continuing the same systemic therapy. The study authors evaluated clinician- and patient-reported outcomes to determine the proportion of patients who did not achieve pre-defined targets based on expert guidelines. From the study, an inadequate response was defined as not achieving a vIGA-AD score of ≤2, a 50% improvement in Body Surface Area (BSA), and a ≥4-point reduction in the Worst Pruritus Numeric Rating Scale (WP-NRS). An optimal response was defined as a vIGA-AD score ≤1 (clear or almost clear skin), BSA ≤2%, and WP-NRS itch score of 0/1 (complete or almost complete itch resolution).
Out of the 2107 total patients with moderate to severe AD, 445 were included based on study criteria. The majority of patients were adults (63.8%), female (62.0%), and Non-Hispanic White (45.4%), with an average age of 31 years. Most patients (92%) initiated treatment with AST, including dupilumab as the most common systemic therapy used (86.5%). The mean vIGA-AD was 3.3 for AST and 3.6 for CST at initiation (P<0.01). The mean worst itch score at baseline was 7.6.
At 6 months, 37% and 67% of AST-treated patients had inadequate responses related to skin clearance and itch outcomes, respectively, and 82% and 79% of patients did not achieve optimal responses. At 12 months, approximately 30% and 67% of AST-treated patients had inadequate responses, respectively, and 85% and 88% of patients did not achieve optimal responses, respectively. According to the authors, CST-treated patients had similar results.
For patients who started an AST on or after September 21, 2021, when 3 new options (tralokinumab, upadacitinib, and abrocitinib) became available, the percentage of patients showing an inadequate control over 12 months was similar to the overall AST cohort, indicating therapeutic inertia despite availability for newer advanced systemic treatment alternatives.
Eichenfield et al’s analysis found that a significant proportion of patients with moderate to severe AD do not achieve adequate disease control with systemic therapies over 3 to 12 months of continuous use. “These findings suggest a need for more proactive management strategies in AD treatment,” concluded the authors.
"This is the first study to assess therapeutic inertia in moderate-to-severe atopic dermatitis. It's crucial for clinicians to consider changing or adjusting the treatment strategy when patient outcomes are unsatisfactory. Engaging in effective dialogue with patients and documenting itch and skin lesion outcomes are key steps in monitoring progress toward treatment goals," said Christopher Bunick, MD, PhD, associate professor of dermatology and physician-scientist at the Yale School of Medicine in New Haven, Connecticut.
Reference
Eichenfield L, Grada A, Knapp K, Munoz B, Crawford J, Silverberg J. Persistent inadequate disease control and therapeutic inertia in moderate to severe atopic dermatitis: a 12-month longitudinal analysis of real-world outcomes from TARGET-DERM registry. Poster presented at: 2023 Revolutionizing Atopic Dermatitis Virtual Conference; December 10, 2023.






