- Case-Based Roundtable
- General Dermatology
- Eczema
- Chronic Hand Eczema
- Alopecia
- Aesthetics
- Vitiligo
- COVID-19
- Actinic Keratosis
- Precision Medicine and Biologics
- Rare Disease
- Wound Care
- Rosacea
- Psoriasis
- Psoriatic Arthritis
- Atopic Dermatitis
- Melasma
- NP and PA
- Skin Cancer
- Hidradenitis Suppurativa
- Drug Watch
- Pigmentary Disorders
- Acne
- Pediatric Dermatology
- Practice Management
- Prurigo Nodularis
- Buy-and-Bill
Article
Atopic dermatitis in elderly common, hard to treat
Author(s):
Adults 60 years and older tend to have a distinct atopic dermatitis presentation and important comorbidities, but dermatologists treating these patients find lacking evidence on how to diagnose and best treat atopic dermatitis in the elderly, according to a recent review.
Atopic dermatitis affects an estimated 2% to 3% of elderly people. And while adults 60 and older tend to have a distinct atopic dermatitis presentation and important comorbidities, dermatologists treating these patients find lacking evidence on how to diagnose and best treat atopic dermatitis in the elderly, according to a review published March 21, 2019 in the British Journal of Dermatology.
RELATED: Get to know the investigator of this study, Anna De Benedetto, M.D.
“Elderly patients with [atopic dermatitis] rarely achieve complete disease remission, and many affected patients eventually die with the condition,” write Anna De Benedetto, M.D., and colleagues at University of Florida College of Medicine, Gaineseville, Fla.
CURRENT RESEARCH
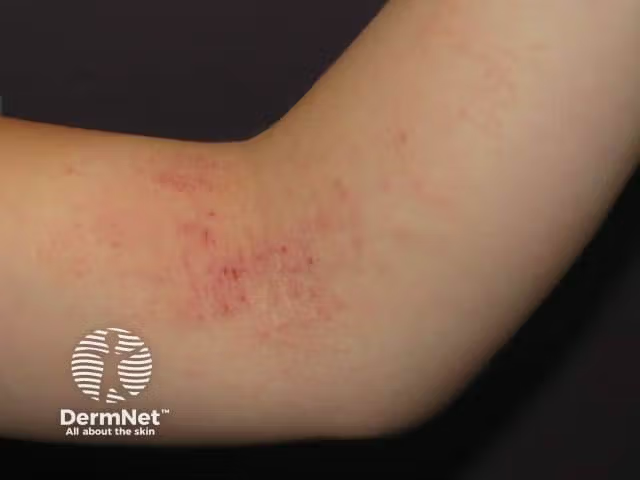
Elderly atopic dermatitis patients tend to present with the reverse sign of lichenified eczema at the antecubital and popliteal fossae, according to the review.
Aging, alone, likely results in pathophysiologic changes that could trigger or worsen atopic dermatitis.
There’s strong evidence that physical or environmental irritation, along with a defective aged epidermal barrier might contribute to the development of atopic dermatitis in elderly patients. The reduction in skin barrier function associated with getting older can exacerbate atopic dermatitis. And older skin has a harder time repairing itself than young skin does.
Immune system changes that occur with age seem linked to atopic dermatitis-associated defects but studies haven’t proven whether those changes directly impact atopic dermatitis pathogenesis. Questions remain about whether an aged immune system might be less able to defend against pathogens, making the elderly more vulnerable to severe and chronic infections, or if the decline in innate immune cell function that comes with age might increase challenges of treating or curing elderly atopic dermatitis patients.
Pruritis, a common and distressing atopic dermatitis symptom, affects a quarter of U.S. patients older than 65 years, in general, who are seen in outpatient clinics. Pruritis, often secondary to xerosis, is associated with atopic dermatitis and other conditions in the elderly. It’s not yet clear if pruritus directly impacts atopic dermatitis pathogenesis in the elderly, according to the review.
More research is needed to look at aging’s effect on the microbiome and how it might impact atopic dermatitis pathogenesis.
“Increased [atopic dermatitis] severity in the elderly may be related to greater S. aureus colonization and infection due to its role in [atopic dermatitis] development in the general population,” write the authors.
Environment also plays a role, but a slightly different role in many elderly atopic dermatitis patients.
Elderly people with atopic dermatitis tend to be most allergic to pollens and dust mites and less sensitive to foods, fungi and animal dander. These older patients often are hypersensitive to fragrance mixes and metals, such as nickel and cobalt, the authors write.
RELATED: Desire for clearance high in atopic dermatitis patients
DIAGNOSING AD IN THE 60 AND OLDER PATIENT
Dermatologists might find it difficult to diagnose atopic dermatitis in elderly patients because these patients tend to have more comorbidities and side effects, including pruritus and xerosis, from medications.
“Currently, older patients are diagnosed with atopic dermatitis after at least six months of symptom assessment and exclusion of other conditions, including cutaneous T cell lymphoma, allergic contact dermatitis, drug reactions, and chronic idiopathic or secondary erythroderma,” according to the authors.
Dermatologists and others treating these patients need clearer diagnostic criteria, according to the review.
CONSIDERATIONS FOR TREATING AD IN ELDERLY
Much about how to best treat atopic dermatitis in 60 and older patients remains unclear. It’s a challenge to treat elderly patients according to standardized guidelines for general atopic dermatitis treatment because dermatologists and others need to consider comorbidities and medications these patients might already be taking. Some examples: Dermatologists might limit cyclosporine use on patients with hypertension and reduced kidney function or limit systemic steroid use in patients with osteoporosis. Elderly patients have an increased propensity for infection, which might cause dermatologists to limit systemic immunosuppressant drugs. And skin thinning and diffuse photoaging might cause doctors to limit even topical steroid treatment in these patients.
These patients might be candidates for biologic medications, including dupilumab. The problem is adult clinic trials for medications like these usually only enroll adults up to age 65.
RELATED: Diagnosing adult-onset atopic dermatitis
MORE RESEARCH NEEDED
Many studies and clinical guidelines addressing atopic dermatitis don’t include the elderly or distinguish adults 60 years and older as a separate population with its own characteristics and needs. Doing so will become more important as the worldwide elderly population expands and the burden of “this relatively undescribed” disease increases, according to the authors. Â
References:
1. Williamson S, Merritt J, De benedetto A. Atopic dermatitis in the elderly: a review of clinical and pathophysiological
hallmarks. Br J Dermatol. 2019;.